The shift in behavioral healthcare delivery has accelerated rapidly over the past few years. What was once a predominantly clinic-based model has expanded into digital-first care environments, prompting organizations to rethink both care delivery and the behavioral healthcare software that supports it.
At the center of this shift is an important decision: telehealth vs in-person behavioral care software. Choosing the right approach is no longer just a clinical consideration. It is a strategic technology decision that affects scalability, patient experience, and operational efficiency.
Whether you are building a new mental health platform or upgrading existing systems, understanding these differences is essential.
Quick Stat:
Telehealth has become mainstream, with 100% of healthcare organizations either offering or planning to offer virtual care services, according to a Teladoc Health Benchmark Survey.
Understanding Telehealth Behavioral Care Software
Telehealth behavioral care software refers to digital platforms that enable remote mental health services through secure, real-time, and asynchronous communication.
These systems are designed to support virtual interactions between patients and providers without requiring physical presence.
Key Capabilities
- Video consultations and teletherapy sessions
- Secure messaging and asynchronous communication
- Remote patient monitoring and engagement tools
- Digital documentation and e-prescriptions
- Mobile and web-based patient portals
Modern mental health telehealth software goes beyond video calls. It enables continuous care, allowing therapists to track patient progress, share resources, and maintain engagement between sessions.
Who Uses It
- Mental health startups
- Online therapy platforms
- Clinics offering hybrid care
- Independent therapists
The rise of teletherapy software has made mental healthcare more accessible, especially for patients in remote or underserved areas.
Quick Stat:
More than 20% of adult patients reported having a telehealth visit in 2022, according to data from the U.S. Census Bureau published by HHS. This highlights how telehealth is not just a growing trend, but an actively used care model across a large patient population.
What Is In-Person Behavioral Care Software?
In-person behavioral care software refers to traditional systems designed for clinic-based care delivery. These platforms focus on managing workflows within physical healthcare settings.
They are typically built around structured clinical operations.
Core Components
- Electronic Health Records (EHR/EMR)
- Appointment scheduling systems
- Billing and insurance processing
- Clinical documentation tools
- Practice management systems
These systems are often categorized under behavioral health EHR software, which is optimized for mental health workflows such as therapy notes, treatment plans, and compliance tracking.
Key Characteristics
- Designed for on-site care delivery
- Heavily reliant on administrative workflows
- Focused on documentation and compliance
- Integrated with insurance and billing systems
While effective for traditional care models, these systems were not originally built for remote-first interactions.
Telehealth vs In-Person Behavioral Care Software: Core Differences
When comparing Telehealth vs in-person behavioral care software, the differences go beyond just location. They fundamentally affect how care is delivered, managed, and scaled.
1. Care Delivery Model
- Telehealth systems support remote, flexible care
- In-person systems are designed for physical clinic visits
Telehealth enables care without geographical limitations, while in-person systems are tied to facility capacity.
2. User Experience
- Telehealth platforms prioritize patient self-service and convenience
- In-person systems rely more on staff-managed workflows
A virtual behavioral health platform typically includes features like self-booking, reminders, and mobile access, enhancing patient engagement.
3. Workflow Structure
- Telehealth supports both real-time and asynchronous care
- In-person care is appointment-driven and sequential
Telehealth allows flexibility, such as follow-ups via chat, while traditional systems require scheduled visits for most interactions.
4. Infrastructure Requirements
- Telehealth systems are cloud-based and device-agnostic
- In-person systems depend on clinic infrastructure and hardware setups
This makes telehealth easier to scale across regions.
5. Scalability
- Telehealth platforms can scale rapidly with minimal physical expansion
- In-person systems require investment in physical locations and staff
This is one of the biggest differentiators in modern behavioral healthcare software comparison discussions.
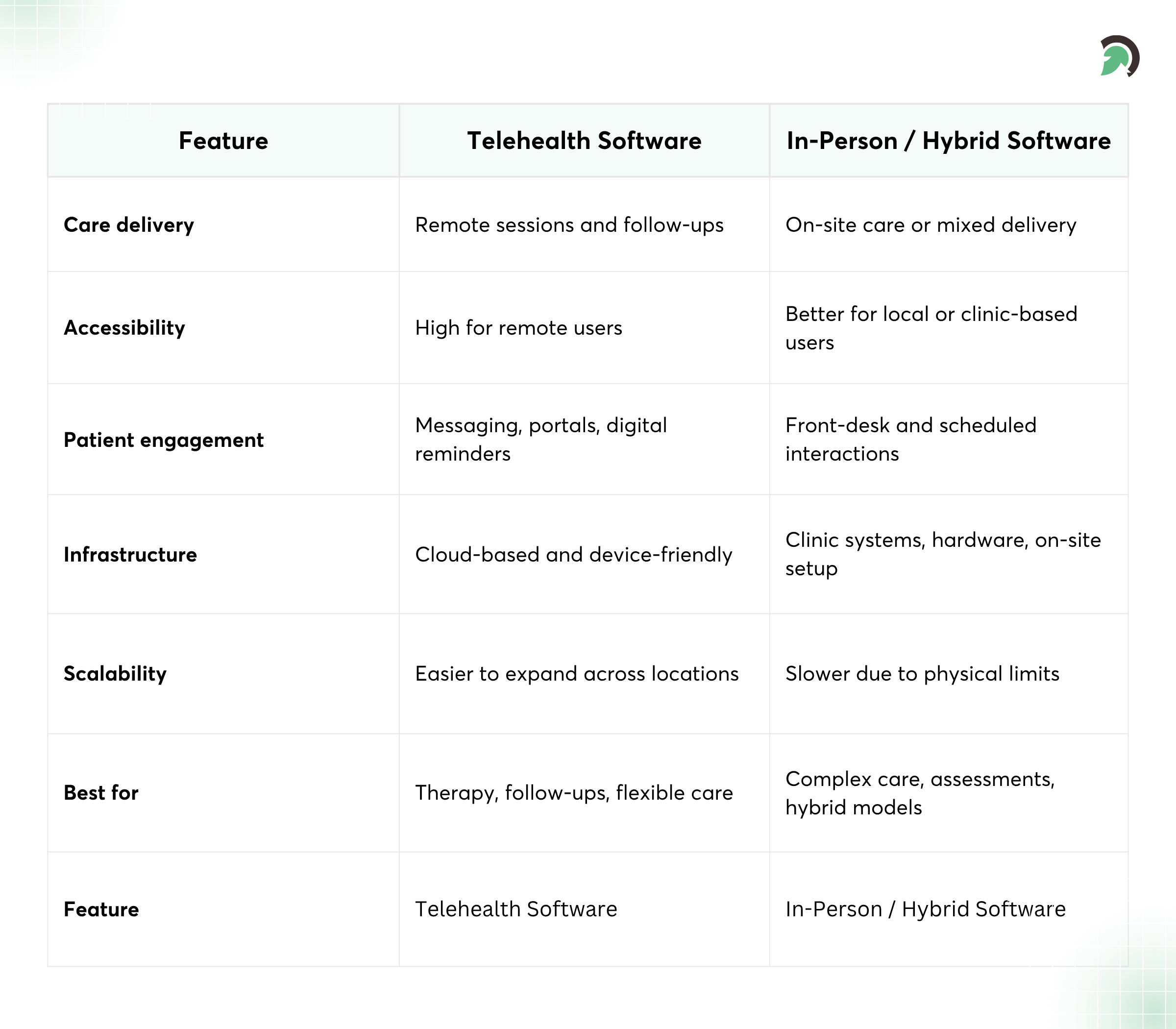
Telehealth vs In-Person vs Hybrid Behavioral Care
Feature Comparison: Telehealth vs In-Person Software
A detailed feature comparison helps clarify how each system supports behavioral healthcare delivery.
Telehealth Software Features
- Video conferencing and teletherapy tools
- Secure messaging
- Digital intake and onboarding
- Remote documentation
- Mobile-first patient access
In-Person Software Features
- Appointment scheduling and calendar management
- Insurance and billing workflows
- Clinical documentation templates
- Compliance tracking
- Integration with lab systems and on-site tools
Key Differences at a Glance
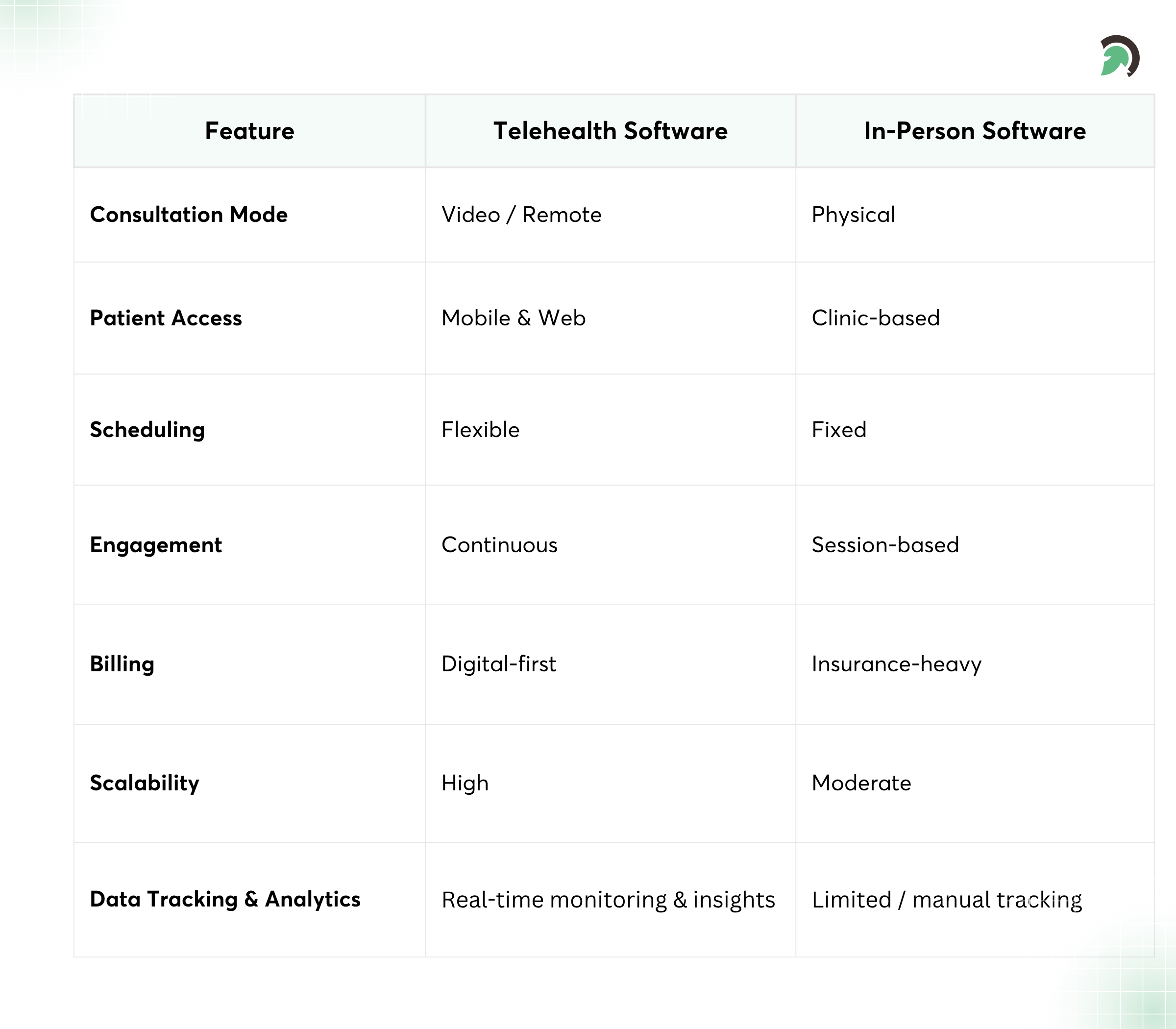
Comparing Telehealth and In-Person Software Features
Many modern systems now combine both capabilities, but the underlying architecture still differs significantly.
Benefits of Telehealth Behavioral Care Software
The adoption of telehealth behavioral care software has been driven by both patient demand and operational efficiency.
- Increased Accessibility: Patients can access care from anywhere, removing geographic barriers.
- Cost Efficiency: Reduced overhead costs for clinics and reduced travel expenses for patients.
- Scalability: Providers can serve more patients without expanding physical infrastructure.
- Continuous Patient Engagement: With features like messaging and follow-ups, care extends beyond scheduled sessions.
- Flexibility for Providers: Therapists can manage schedules more efficiently and offer flexible session timings.
These advantages have made mental health telehealth software a critical component of modern behavioral healthcare systems.
Quick Stat:
Telehealth has become a standard part of care delivery, with about 95% of HRSA-funded health centers using telehealth services in 2024, according to the U.S. Department of Health & Human Services (HHS).
Benefits of In-Person Behavioral Care Software
Despite the growth of telehealth, traditional systems remain essential.
- Better for Complex Cases: Severe mental health conditions often require in-person evaluation.
- Stronger Therapeutic Connection: Face-to-face interaction can improve communication and trust.
- Physical Observation: Providers can assess non-verbal cues more effectively.
- Structured Clinical Workflows: Established processes ensure compliance and consistency.
- Integrated Insurance Workflows: In-person systems are often better aligned with traditional billing processes.
Limitations of Each Approach
Understanding limitations is key to making the right decision.
Telehealth Software Challenges
- Dependence on the internet and devices
- Privacy and data security concerns
- Not ideal for crisis or emergency situations
In-Person Software Challenges
- Limited scalability
- Higher operational costs
- Restricted patient reach
These trade-offs are central to the Telehealth vs in-person behavioral care software decision-making process.
Effectiveness: What Does the Data Suggest?
Studies and industry insights consistently show that telehealth is effective for many mental health conditions, including anxiety, depression, and mild behavioral disorders.
However, in-person care remains critical for:
- Crisis intervention
- Severe psychiatric conditions
- Cases requiring physical evaluation
This reinforces the idea that both systems have their place in modern care delivery.
The Rise of Hybrid Behavioral Care Platforms
One of the most important trends in behavioral healthcare is the shift toward hybrid systems.
Instead of choosing between telehealth and in-person care, organizations are adopting platforms that support both.
What Hybrid Systems Offer
- Unified patient records
- Flexible care delivery (remote + in-person)
- Seamless transitions between care modes
- Improved patient outcomes
A well-designed hybrid system combines the strengths of both approaches, making it the preferred model for many providers.
How to Choose the Right Software
Choosing the right behavioral care software depends on your care model, patient needs, operational priorities, and long-term growth plans. Some providers need a telehealth-first solution to improve access and flexibility, while others require stronger in-person workflows for evaluations, documentation, and structured treatment delivery. Many organizations now prefer hybrid platforms that support both virtual and in-person care, giving them more flexibility as patient expectations and service models continue to evolve.
When comparing solutions, it helps to evaluate the platform from both a clinical and operational perspective. The right software should not only support how care is delivered today, but also help your organization scale efficiently, maintain compliance, and improve the overall patient experience.
Key factors to consider include:
- Type of care you provide: Therapy-focused and follow-up care often align well with telehealth platforms, while complex psychiatric services may need in-person or hybrid workflows.
- Patient demographics: Younger and digitally comfortable patients may prefer virtual care, while some users still value face-to-face interactions.
- Practice size and expansion goals: Smaller practices may prioritize affordability and ease of use, while larger organizations often need scalability, multi-location access, and broader integrations.
- Compliance and security needs: The software should support HIPAA and other relevant privacy, security, and documentation requirements.
- Features and system integrations: Look for scheduling, documentation, billing, reporting, teletherapy tools, and compatibility with other healthcare platforms.
- Long-term flexibility: A system that can support both current operations and future growth will reduce disruption as your care model changes.
The best choice is the one that fits your clinical workflows, supports your team, and creates a better experience for patients across every stage of care.
Key Features to Look for in Behavioral Care Software
Regardless of the model, certain features are essential.
- Secure and compliant infrastructure
- Integrated teletherapy capabilities
- Billing and insurance support
- Analytics and reporting
- Interoperability with third-party systems
If you are evaluating the best behavioral health software for telehealth, prioritize platforms that offer both usability and scalability.
Technology Considerations for Software Development
When building or selecting a system, technical architecture plays a major role.
Telehealth Systems Require:
- Real-time video infrastructure
- Cloud-based scalability
- Mobile optimization
- API integrations
In-Person Systems Require:
- Robust data management
- Integration with clinical systems
- Secure on-premise or hybrid infrastructure
Organizations investing in behavioral healthcare software development must carefully evaluate these requirements.
Custom-built solutions often offer greater flexibility than off-the-shelf tools.
The Role of Teletherapy Software in Modern Care
Teletherapy software has become an essential part of modern behavioral health delivery, helping providers offer care beyond the traditional clinic setting. As remote care adoption continues to grow, these platforms are making it easier for therapists, counselors, and behavioral health organizations to deliver accessible, flexible, and consistent support to patients.
Teletherapy software typically supports:
- One-on-one virtual therapy sessions
- Group therapy and shared counseling sessions
- Progress tracking and treatment monitoring
- Secure resource sharing and follow-up communication
More advanced platforms may also include scheduling, documentation, patient engagement tools, and integrations with broader behavioral health systems. With the increasing demand for remote care, teletherapy platforms are no longer limited to video consultations alone. They are evolving into more complete digital care ecosystems that support ongoing communication, care continuity, and better patient experiences.
Future Trends in Behavioral Healthcare Software
The industry is evolving rapidly, with several emerging trends shaping the future.
- AI-Powered Insights: Predictive analytics for patient behavior and treatment outcomes.
- Personalized Care Platforms: Tailored treatment plans based on patient data.
- Remote Monitoring Tools: Wearables and digital tracking for continuous care.
- Expansion of Hybrid Models: More organizations are adopting flexible care delivery systems.
- Platform Consolidation: Unified systems combining EHR, telehealth, and analytics.
These trends are redefining how Telehealth vs in-person behavioral care software is approached, shifting the focus toward integrated ecosystems.
Conclusion
There is no one-size-fits-all answer when comparing Telehealth vs in-person behavioral care software. Each approach offers unique advantages and serves different clinical and operational needs.
Telehealth systems provide scalability, accessibility, and flexibility, making them ideal for expanding care delivery. In-person systems, on the other hand, offer depth, structure, and effectiveness for complex cases.
The future lies in hybrid solutions that combine the strengths of both.
For organizations looking to build or upgrade their systems, investing in the right technology is critical. Whether you need a scalable virtual behavioral health platform, advanced mental health software, or a robust clinic-based system, the right development approach can make all the difference.
At EvinceDev, we specialize in behavioral healthcare software development, helping organizations design and build secure, scalable, and high-performance digital health platforms tailored to modern care delivery needs.




