Key Takeaways:
- Trust First Design: Build user-centric interfaces that prioritize comfort, clarity, and ease of use to improve patient trust and platform adoption.
- Strong Data Security: Implement encryption, access controls, and secure authentication to protect sensitive health data and ensure compliance.
- Compliance Matters: Follow HIPAA, GDPR, and local regulations from the start to avoid risks and build a legally compliant platform.
- Seamless UX Flow: Design smooth onboarding, scheduling, and session flows to reduce friction and improve patient engagement.
- Scalable Architecture: Use cloud-based infrastructure that supports growth in users, sessions, and data without affecting performance.
- Reliable Video: Care Ensure high-quality, stable video sessions to maintain trust and deliver consistent virtual therapy experiences.
- Smart Integrations: Integrate EHRs, payments, and APIs to streamline workflows and improve operational efficiency across systems.
- Continuous Improvement: Use analytics and feedback to refine features, enhance user experience, and improve long-term platform outcomes.
If you’re exploring a tele-behavioral health platform, you’re probably trying to solve a real problem: getting quality mental care to people who can’t easily reach it. The right tele-behavioral health platform development service can turn that goal into a secure, scalable product that supports clinicians, engages patients, and stays compliant as you grow. In this guide, I’ll walk you through what these platforms are, what to build, how development typically works, and where modern teams are seeing the biggest wins.
What is Tele-Behavioral Health?
Tele-behavioral health is the remote delivery of mental and behavioral healthcare services designed to fit naturally into a patient’s life. Instead of expecting someone to travel, wait in a lobby, and coordinate time off work, care can happen from home, a clinic room, or anywhere with a secure connection.
Most platforms support a combination of:
- Therapy and counseling sessions (individual and group)
- Clinical monitoring and check-ins
- Consultations with licensed providers
Why Tele-Behavioral Health is Growing
Demand isn’t just increasing, it’s changing how healthcare services are planned. A few strong drivers are pushing adoption forward:
- Accessibility: Remote care is especially valuable for rural and underserved communities.
- Convenience: Patients can reduce travel, time costs, and scheduling friction.
- Post-pandemic digital transformation: Many organizations now treat virtual care as a permanent capability rather than a temporary workaround.
Role of Platform Development Services
This is where a tele-behavioral health platform development service becomes the difference between “we have a video call” and “we have a real care system.” A professional build helps you create a secure and compliant virtual care environment that works for everyone involved.
A good platform development team typically focuses on:
- Security and compliance (not just encryption, but the processes around it)
- Scalability for growth in users, sessions, and data volume
- Workflow support for clinicians, patients, and administrators
What is the Tele-Behavioral Health Platform Development Service?
Definition and Scope
A tele-behavioral health platform development service is an end-to-end product development for digital mental healthcare delivery. It covers building the full system across web, mobile, and cloud-based components so your platform isn’t held together with add-ons.
Scope usually includes:
- Frontend experiences (patient and provider)
- Backend services and integrations
- Cloud hosting and operational monitoring
- Testing, deployment, and ongoing maintenance
Key Objectives
Most teams start with high-level goals, but the best teams translate those goals into measurable functionality. Typical objectives include:
- Improving access to mental healthcare through scheduling, messaging, and seamless sessions
- Enhancing patient engagement with reminders, progress tracking, and guided support
- Ensuring secure data handling with privacy controls, auditability, and strict access policies
Difference from General Telehealth Platforms
A general telehealth platform can support basic virtual visits, but mental health care has a unique workflow and privacy needs. For example, a behavioral health platform often requires therapy-focused features, session documentation flow, and stronger consent and confidentiality patterns.
In practice, behavioral health telehealth software tends to include:
- Therapy-first workflows (treatment planning, session notes, follow-ups)
- Enhanced privacy and compliance controls
- Clinical tools that support documentation and care continuity
Types of Tele-Behavioral Health Platforms
Video Therapy Platforms
These are the most recognizable tele-mental health platform development builds: secure video sessions that support one-on-one and group therapy. When the video experience is unreliable, patient trust drops quickly so quality and controls matter.
Key capabilities typically include:
- Secure video conferencing with session recording controls
- Group session support with moderator tools
- Session start/end flows that reduce clinician friction
Remote Patient Monitoring Systems
Remote monitoring focuses on tracking mental health indicators over time. Instead of waiting for the next appointment, care teams can see trends and respond earlier.
Common elements include:
- Dashboards for clinicians to review monitoring signals
- Integration with wearable devices and patient-reported data
- Automated alerts for risk indicators (according to your clinical rules)
Mental Health Mobile Applications
Mobile apps often serve as a “support layer” around therapy, providing self-care and between-session guidance. Many teams treat mental health app development as a retention and engagement strategy, not just a feature.
Popular app features include:
- Mood tracking and journaling
- Guided exercises and psychoeducation content
- AI-based suggestions (when used responsibly and transparently)
Integrated Behavioral Health Systems
Integrated systems combine EHR, billing, and telehealth into a centralized platform for clinics and provider groups. This is often the path when you want to reduce operational complexity and unify patient data.
- Centralized workflows for providers
- Unified records and documentation
- Streamlined billing and reporting
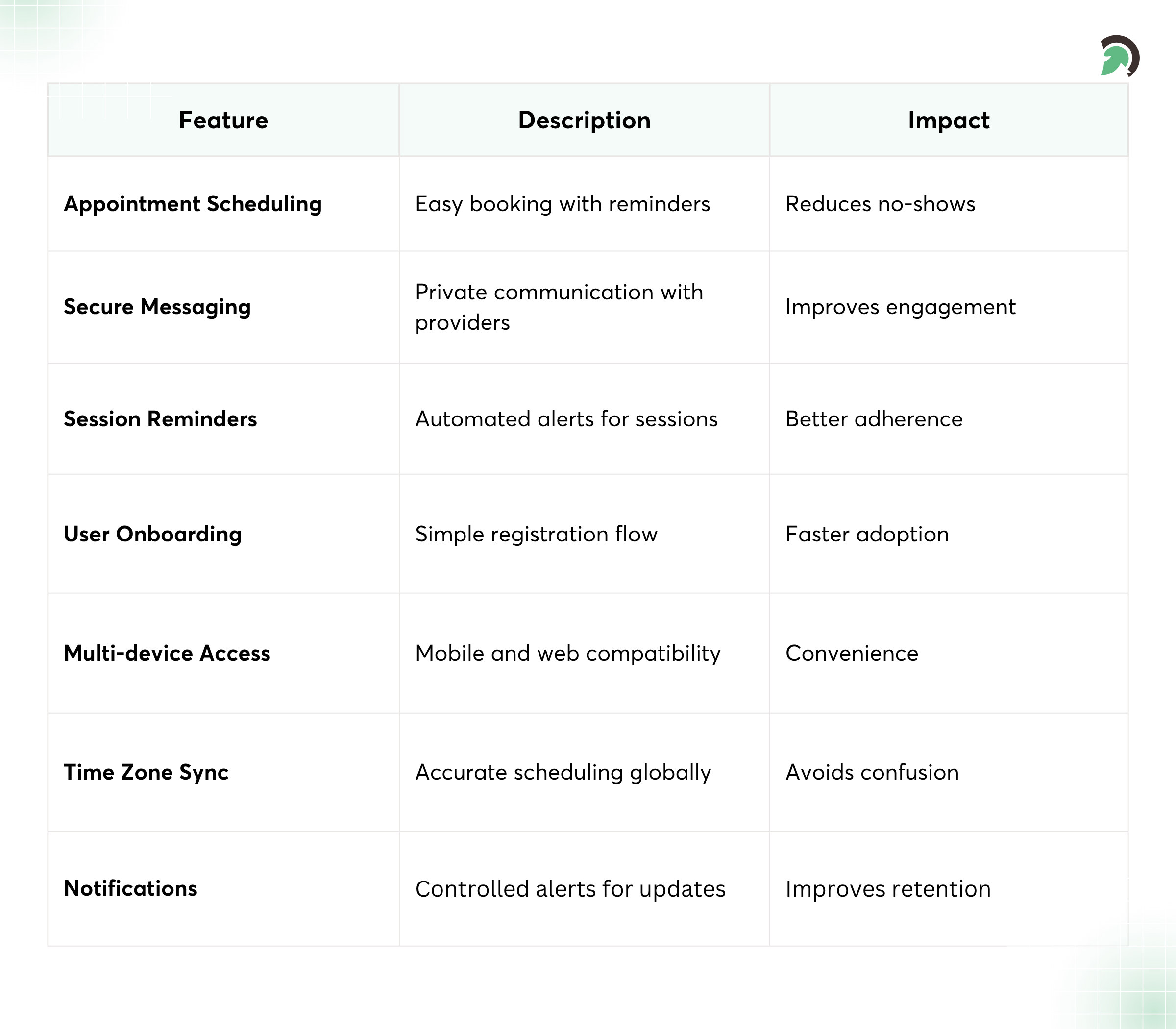
Core Features of Tele-Behavioral Health Platforms
Patient-Side Features
Appointment scheduling
Scheduling should feel effortless. Patients are already managing emotions, work, caregiving, and stress so your platform should remove avoidable steps.
Look for features like:
- Easy onboarding
- Session reminders
- Clear time zones and appointment confirmations
Secure messaging
Secure messaging enables continuity between sessions. Done well, it reduces no-shows and keeps patients from feeling like they’re “waiting silently.”
Practical considerations include:
- Message threading and clinician visibility rules
- Attachments support (when clinically appropriate)
- Notifications that respect privacy and reduce anxiety
Provider-Side Features
Session management dashboard
Clinicians need clarity fast: who’s waiting, what’s scheduled, what documentation is due, and what follow-up actions matter.
Dashboards commonly include:
- Session queues and status indicators
- Clinical task lists tied to appointments
- Quick access to patient history relevant to care
Clinical documentation tools
Great documentation tools reduce time spent on admin work and increase time spent on patient care. This is a place where virtual therapy platform development efforts pay off.
- Treatment planning support
- Session notes workflows
- Notes automation where appropriate (with clinician review and control)
Admin Features
User and role management
Every organization needs precise permissions. Role-based access control ensures that staff see only what they’re authorized to handle.
Billing and reporting
Operational visibility matters. Admin tools should support:
- Claims workflows and billing tracking
- Reporting by provider, clinic, or program
- Auditability for compliance
Analytics and performance dashboards
Once your tele-behavioral health platform grows, you’ll want to understand usage patterns: appointment completion rates, messaging responsiveness, retention, and session quality trends. Analytics helps you iterate on both product and care processes.
Advanced Features
AI-powered insights
AI can support mental healthcare, especially through summarization, trend detection, and decision support. The goal isn’t to “replace a clinician,” but to make care more efficient and consistent.
Chatbots for patient support
Chatbots can reduce repetitive questions (like appointment steps or platform navigation) so your team can focus on clinical tasks. When used, they should be transparent, safe, and designed to route users to humans when needed.
Predictive analytics for risk detection
Some platforms apply predictive analytics to identify elevated risk signals. This kind of capability should be built with careful governance, clear clinical interpretation, and strong privacy protections.
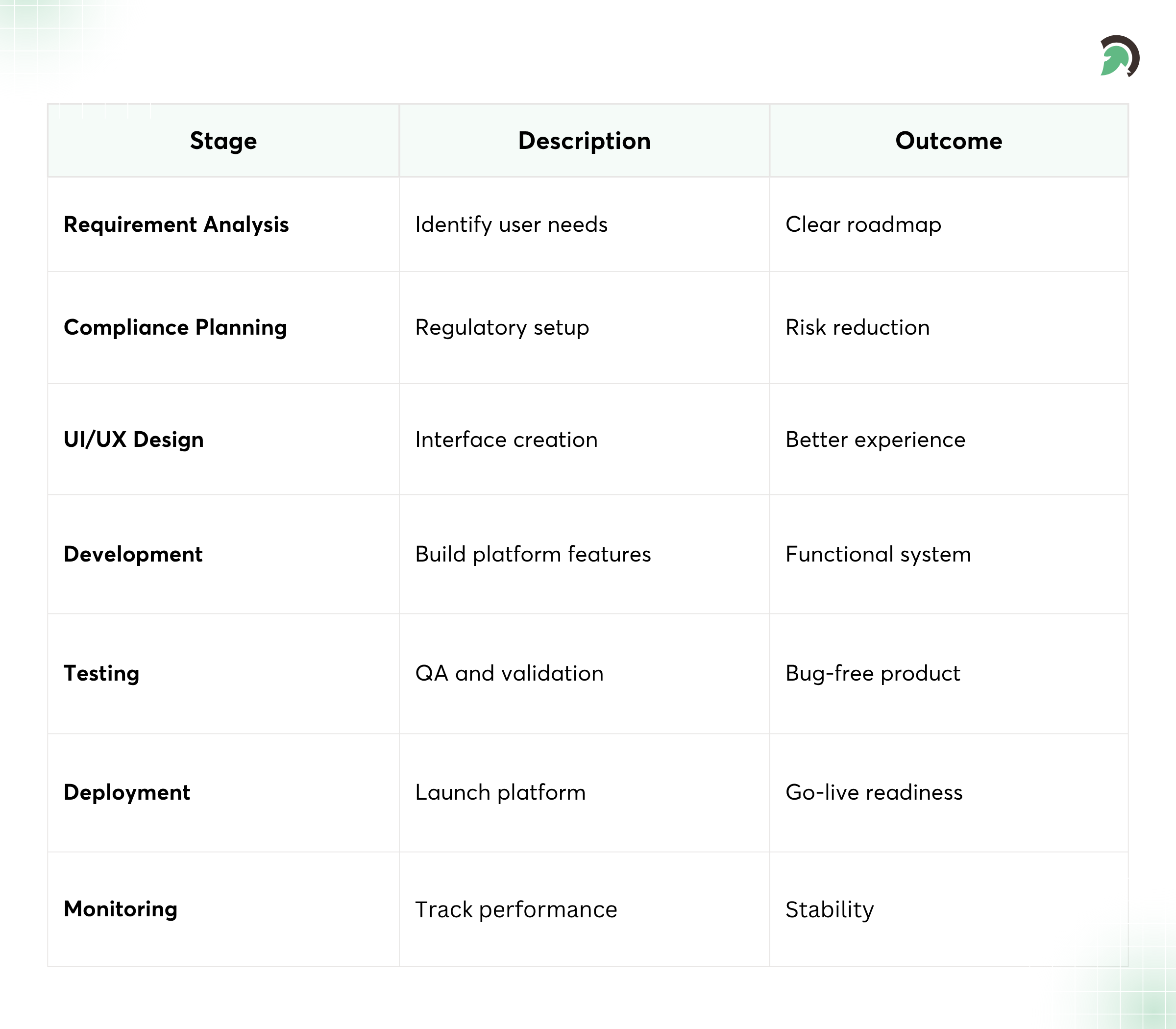
Tele-Behavioral Health Platform Development Process
Step 1: Requirement Analysis
Start by mapping real workflows not just features. Identify:
- Target users (patients, clinicians, admins)
- Key journeys (onboarding, scheduling, session flow, follow-up)
- Clinical and operational needs that drive product decisions
Step 2: Compliance Planning
Compliance planning must happen early, because it affects architecture, data flows, and product UX. Teams typically plan for:
- HIPAA in the USA
- GDPR in EU contexts
- Regional healthcare regulations relevant to your users
Step 3: UI/UX Design
UI/UX should support both patient comfort and clinician efficiency. A patient-friendly interface reduces drop-offs; a clinician-focused interface reduces admin burden.
- Simple onboarding and session reminders
- Clinician dashboards that minimize clicks
- Accessibility considerations for wider adoption
Step 4: Development Phase
This is the build stage where product becomes real. You’ll typically split work into frontend, backend, and integration tasks.
- Frontend and backend development
- API integrations and cloud infrastructure
- Video and messaging components (where applicable)
Frontend and backend development
The frontend controls the experience; the backend handles security, data integrity, and business logic. Together, they determine whether your tele-behavioral health platform feels reliable in daily use.
API integrations and cloud infrastructure
Integrations with EHR systems, payments, and video APIs often define launch timelines. Planning early helps avoid surprises late in the project.
Step 5: Testing and QA
Testing isn’t optional for healthcare platforms. It’s how you protect users and reduce risk before release.
- Security testing
- Performance validation (latency, session quality, load)
- Usability testing across devices and roles
Step 6: Deployment and Maintenance
Deployment is the start, not the finish. Successful teams set up continuous updates and monitoring to keep the platform secure, stable, and aligned with evolving needs.
- Operational monitoring and alerting
- Regular security and performance reviews
- Feature improvements based on real usage
Security and Compliance Requirements
Key Regulations
Security and compliance aren’t “checklist items” they influence design decisions all the way through development.
- HIPAA (USA)
- GDPR (EU)
- Local healthcare regulations relevant to where your users are located
Security Measures
- Data encryption (in transit and at rest)
- Secure authentication flows
- Role-based access control and audit logs
Role-based access control and audit logs
Audit logs are especially important for healthcare environments. They help you trace access and understand what happened when something needs review.
Data Privacy Considerations
- Consent management workflows
- Data storage and retention policies
- Clear rules for what data is shared, with whom, and why
Benefits of Tele-Behavioral Health Platform Development
For Healthcare Providers
- Improved operational efficiency
- Wider patient reach beyond geographic limitations
For Patients
- Easy access to care without a long travel
- Reduced stigma and more control over where support happens
For Organizations
- Scalable healthcare delivery models
- Cost optimization through streamlined operations and reduced no-show friction
Challenges in Tele-Behavioral Health Platform Development
-
Regulatory Complexity
Compliance varies by region and use case. Even if your product is “globally available,” your workflows may still need region-specific handling.
-
Data Security Risks
Because behavioral health data is sensitive, security expectations are higher. A single weak point, like overly broad permissions or weak audit trails, can become a major risk.
-
Integration with Existing Systems
Connecting to EHRs, billing systems, and internal clinic tools can be slow if requirements aren’t defined early. Many projects succeed or struggle based on integration planning.
-
User Adoption Barriers
Patients and clinicians won’t use a platform that feels confusing or unreliable. If the onboarding is heavy, notifications are unclear, or sessions frequently fail, adoption will stall.
Cost of Tele-Behavioral Health Platform Development
Key Cost Factors
Pricing varies widely, but the main cost drivers are consistent. Expect cost to depend on:
- Feature complexity: video, messaging, monitoring, AI features, admin tooling
- Compliance requirements: governance, security controls, auditability
- Development team size: product design, engineering, QA, DevOps
If you’re budgeting, it helps to define a phased roadmap (MVP first, then advanced features). That approach reduces risk and makes future investment easier to justify.
Latest Trends in Tele-Behavioral Health Platforms
-
AI in Mental Healthcare
AI is increasingly used for documentation support, personalization, and operational efficiency. The most credible teams build AI with guardrails, clinician control, explainability, and safe escalation paths.
-
Virtual Therapy Enhancements
Video therapy is evolving beyond “calls.” Better session tools, smoother onboarding, and more structured treatment workflows are becoming standard expectations in the market.
-
Wearable Integration
Wearables can support monitoring by capturing passive signals and trends. When paired with patient-reported data, they can help clinicians better understand changes over time.
-
Personalized Treatment Plans
Personalization is shifting from generic recommendations to care plans that reflect patients’ histories, goals, and monitoring signals while keeping clinicians at the center of decision-making.
-
Real-Time Data Analytics
Real-time insights help programs act faster: session quality checks, engagement metrics, and risk trend monitoring can all improve outcomes when implemented carefully.
Conclusion
Building a tele-behavioral health platform is not just a tech project; it’s a commitment to safer access, better continuity of care, and a patient experience that respects mental health needs. When you choose a proven tele-behavioral health platform approach, secure architecture, therapy-centered workflows, and clear compliance planning, you create a system people can rely on. Modern wins like monitoring, guided patient support, and thoughtful AI capabilities can help you move from occasional sessions to continuous care.
If you’re planning your next steps, consider exploring how a platform partner like EvinceDev can support your roadmap from discovery through deployment so you can launch with confidence and scale responsibly. The future of behavioral health delivery is digital, but it should also be human. Start building the version that earns trust.



